“Safe and natural.” It’s a marketing phrase attached to dietary supplements that’s often accepted as self-evident. The marketing works. Supplements have a strong health halo. But evidence suggests that this reputation may be undeserved. Not only are there continued questions about whether most supplements have any health benefits whatsoever, there is also evidence that they can be harmful. We can’t even be confident that what’s on the label is actually in the bottle. Just two days ago I was notified of another long list of supplements and remedies that the FDA had identified that were contaminated with prescription drugs. These warnings about products sold as supplements appear regularly. Some time ago I asked, “What’s in your supplement?“, and noted that contamination and poor product quality standards continue to raise questions about whether supplements can be used safely at all, because the harms, when they occur, can be catastrophic. No matter how you feel about their efficacy, we can probably all agree no consumer should lose an organ from taking a health supplement. But it can happen. Continue reading
alternative medicine
The Trojan Horse of “Integrative Medicine” arrives at the University of Toronto

Medicine is a collaborative practice. Hospitals are the best example, where dozens of different health professionals work cooperatively, sharing responsibilities for patient care. Teamwork is essential, and that’s why health professionals obtain a large part of their education on the job, in teaching (academic) hospitals. The only way that all of these different professions are able to work together effectively is that their foundations are based on an important, yet simple, principle. All of us have education and training grounded in basic scientific principles of medicine. Biochemistry, pharmacology, physiology – we all work from within the same framework. As a pharmacist, my role might include working with physicians and nurses to manage and monitor medication use. A team approach is only possible when you’re working from the same playbook, and with the same aim. And in medicine, that playbook is science.
That’s why “integrative” medicine frightens me so much. Integrative medicine is a tactic embedding complementary and alternative medical practices into conventional medical care. Imagine “integrating” a practitioner into the health system that doesn’t accept germ theory. Or basic disease definitions. Or the effectiveness of vaccines. Or even basic biochemistry – perhaps they believe in treatments that restore the body’s “vital force” or manipulate some sort of “energy fields”. Instead of relying on objective signs and symptoms, they base treatments on pre-scientific beliefs, long discarded from medicine. There may be entirely different treatment goals, which are potentially antagonistic to the scientific standard. Imagine a hospital or academic setting where this occurs, and the potential impact on the quality of care that is delivered. Continue reading
The facts about alternative medicine
People have been living on earth for about 250,000 years. For the past 5,000 healers have been trying to heal the sick. For all but the past 200, they haven’t been very good at it.
– Dr. Paul Offit
Twenty years is a long time in medicine. I celebrated my 20th pharmacy class reunion last weekend. Of course reunions are time to reflect back to our early years as pharmacists. Lots has changed. Much of the therapeutics I was taught is now obsolete. In 1993, HIV was a death sentence and there were only three, largely ineffective drugs available. Thanks to new drugs, HIV can now be managed like a chronic disease, and some of my colleagues have HIV-focused pharmacy practices. The same dramatic changes have occurred in fields like cancer, and transplant medicine. And in some cases, the cause of disease has become more clear – my old textbooks make no mention of Helicobacter pylori as a cause of ulcers.
The practice of pharmacy has changed, too. On the positive side, pharmacists are working in new settings where they can focus on medication management, and not just dispensing prescriptions. Regulators are granting pharmacists the ability to take on new roles, and pharmacists are being compensated for more than simply “count, pour, lick and stick.” From that perspective, it’s a promising time to be a pharmacist. But there’s a much more disturbing side to the profession that’s emerging, too. Community (retail) pharmacy practice is under pricing and competitive pressure, and smaller pharmacies are being subsumed into big retailers where the pharmacy department is buried in the back – a loss leader to bring in patients, but hardly with a health-care focus. And most disturbingly, I see a move within retail pharmacy practice to leverage its professional credibility to sell all types of modern-day snake oil, ranging from detox kits and “cleanses” to dubious “food intolerance” testing. Homeopathic remedies (an elaborate placebo system of sugar pills) are increasingly found on pharmacy shelves, alongside real medicine. And don’t forget the enormous wall of vitamins that seems to get larger and larger. Yes, complementary and alternative medicine is booming, and pharmacy wants its share. Pharmacy regulators turn a blind eye. What do my pharmacy colleagues tell me? They’ll tell me it’s customer demand, and that they don’t recommend the quackery. To me, I see this trend as damaging the credibility of pharmacists in the eyes of the public and of other health professionals. Continue reading
Intravenous vitamin injections: Where’s the evidence?
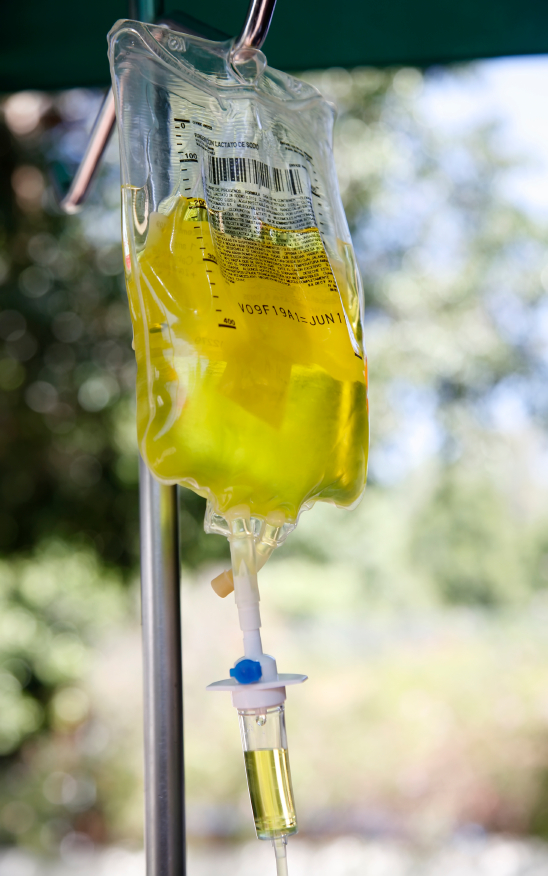
Vitamins are magic. Especially when they’re injected. Roll up the sleeve, find a vein, insert a needle and watch that colourful concoction flow directly into the bloodstream. It may sound somewhat illicit, but that person infusing it is wearing a white coat, and you’re sitting in a chic clinic. There must be something to it, right? Intravenous vitamin injections are popular with celebrities and have even been described by Dr. Oz as “cutting edge”. Advocates claim vitamin injections can benefit serious conditions like cancer, Parkinson’s disease, macular degeneration, fibromyalgia, depression, and that modern-day obsession, “detoxification”. And vitamin infusions aren’t just for the ill. They’re also touted as helpful for preventing illness, too. A search for vitamin injections brings up millions of hits and dozens of advertisements. There is no question that vitamin injections are popular. But despite all the hype and all the endorsements, there is no credible evidence to suggest that routine vitamin infusions are necessary or offer any meaningful health benefit. Vitamin infusions are a marketing creation, giving the illusion you’re doing something for your health, but lacking any demonstrable efficacy. What’s more concerning, providers of vitamin therapies target their marketing at those fighting life-threatening illnesses like cancer, selling unproven treatments in the absence of good scientific evidence that they are beneficial.
The intravenous vitamin industry is a sideshow to science-based health care. Yes, there is an established medical role for injectable vitamins, though it’s no energy-boosting cure-all – they’re used to replace what we should obtain in our diet. As a hospital-based pharmacist I used to prepare sterile bags of total parenteral nutrition (TPN), a mixture of vitamins, carbohydrate, protein and fat that completely replaced the requirement to eat. TPN is effective, but not without risks, and far less preferable than getting your nutrients the old fashioned way – by eating them. There’s also the routine use of injectable vitamins like B12, or iron, all of which can be science-based when used to address true deficiencies, or to manage specific drug toxicities. IV vitamins (particularly thiamine) are also used in the emergency room, given to alcohol-dependent patients in order to prevent Wernicke’s encephalopathy. And there is the therapeutic use of high-dose minerals like intravenous magnesium for acute asthma attacks. But there is no medical justification to infuse vitamins into a vein when you can more appropriately obtain those nutrients in your diet.
Continue reading
Recommended Reading: “The Cure for Everything” and “Which comes first, cardio or weights?”
You may consider yourself a critical thinker and scientific skeptic, but do you have any blind spots? I’ve had a skeptical perspective for a long time (my teenage cynicism wasn’t just a phase) but the framework for my thinking has developed over years. Professionally, the blind spot that the pharmacy profession has towards supplements and alternatives to medicine was only clear after I spent some time working in a pharmacy with thriving homeopathy sales. In looking for some credible evidence to guide my recommendations, I discovered there was quite literally *nothing* to homeopathy. Once I discovered blogs like Respectful Insolence, the critical thinking process, and scientific skepticism, took off from there. Continue reading
Medical Doctors, Unproven Treatments, and Professional Standards
If there’s one group that you’d expect would take a dim view of physician provision of unproven or ineffective treatments, it’s the regulatory colleges that determine medical standards of practice. And that’s why it’s concerning and surprising the College of Physicians and Surgeons of Ontario (CPSO) has published the following draft policy paper, Non-Allopathic (Non-Conventional) Therapies in Medical Practice. The policy as written is unclear with respect to physician expectations. It also appears to significantly diminish the requirement for physicians to provide medical care and advice based on established scientific standards.
To start, let’s look at the CPSO’s role. From their own description:
Doctors in Ontario have been granted a degree of authority for self-regulation under provincial law. The College of Physicians and Surgeons of Ontario is the body that regulates the practice of medicine to protect and serve the public interest. This system of self-regulation is based on the premise that the College must act first and foremost in the interest of the public. All doctors in Ontario must be members of the College in order to practise medicine.
Now let’s take a look at the policy, and its congruence to the CPSO’s role. There’s already been a strong reaction online. Both The Committee for the Advancement of Scientific Skepticism (CASS), as well as Dr. David Gorski, at the Science-Based Medicine Blog have posted detailed analyses. Each identifies multiple shortcomings in the policy that put the public interest into question. Here are some additional thoughts on the policy itself [PDF]. Continue reading



You must be logged in to post a comment.